Anterior cruciate ligament reconstruction surgery restores knee stability after severe injuries. It involves grafting to replace the damaged ligament, improving joint function and reducing instability. This procedure is common among athletes and individuals with high knee demands, aiming to restore full mobility and strength over time. While recovery timelines vary, most patients regain full function within 6–12 months, depending on adherence to rehabilitation and individual factors like age, graft type, and injury severity. Here is a detailed breakdown of the recovery phases and milestones.
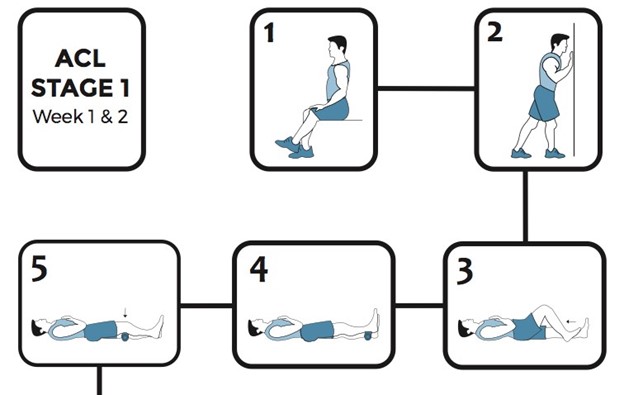
Immediate Post-Surgery Phase (0–2 Weeks)
The first two weeks focus on pain management and reducing swelling:
- Weight-bearing: Crutches are typically required for 1–2 weeks, with gradual progression to full weight-bearing as tolerated.
- Bracing: A knee brace may be used to limit movement and protect the graft.
- Physical therapy (PT): Gentle exercises begin 2–3 days post-surgery to restore knee extension and flexion.
- Pain control: Ice, elevation, and prescribed medications help manage discomfort and inflammation.
Early Rehabilitation Phase (2–8 Weeks)
This phase aims to rebuild mobility and strength:
- Range of motion: Focus on achieving full knee extension and flexion (0–120 degrees) through guided exercises.
- Muscle activation: Quadriceps and hamstring strengthening begins with low-resistance exercises like leg raises and heel slides.
- Gait training: Transitioning off crutches and restoring normal walking patterns.
- Swelling management: Continued use of compression therapy and ice.
Intermediate Phase (2–4 Months)
Patients gradually reintroduce functional movements:
- Strength training: Emphasis on squats, lunges, and cycling to rebuild muscle mass.
- Low-impact cardio: Stationary biking or swimming improves endurance without stressing the knee.
- Balance and proprioception: Single-leg stands and balance board drills enhance joint stability.
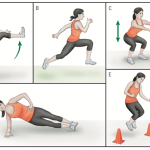
Advanced Phase (4–8 Months)
Preparation for returning to sports or high-demand activities:
- Plyometrics and agility drills: Jumping, cutting, and pivoting exercises reintroduce dynamic movements.
- Sport-specific training: Gradual reintegration into drills relevant to the patient’s sport (e.g., dribbling for basketball players).
- Strength benchmarks: Achieving ≥90% strength in the operated leg compared to the uninjured side.
Return to Activity (8–12 Months)
Full clearance depends on meeting functional criteria:
- Medical clearance: Surgeons often require passing a “return-to-sport” test assessing strength, stability, and agility.
- Psychological readiness: Confidence in the knee’s stability is crucial for athletes.
- Ongoing maintenance: Continued strength training reduces re-injury risk.
Factors Influencing ACL Reconstruction Surgery Recovery
- Graft type: Autografts (patient’s tissue) may heal faster than allografts (donor tissue).
- Age: Younger patients often recover quicker due to better tissue regeneration.
- Adherence to PT: Consistent rehabilitation improves outcomes significantly.
- Pre-surgery preparation: Restoring knee mobility before surgery reduces post-op stiffness.
Risks of Rushing Recovery
Premature return to high-impact activities increases the risk of:
- Graft failure: Stress on the healing ligament can cause re-tears.
- Cartilage damage: Chronic instability may lead to meniscus injuries or osteoarthritis.
Conclusion
ACL reconstruction recovery is a marathon, not a sprint. While timelines vary, most patients resume light activities within 2–3 months and return to sports after 8–12 months. Success hinges on strict adherence to physical therapy and avoiding shortcuts. With patience and discipline, approximately 80% of patients regain full knee function, minimizing long-term complications like osteoarthritis. Always follow your surgeon’s guidance to ensure optimal healing.
For enquiries and online appointments, send a message to
www.DrAyyappanVNair.com/contact
For informative videos related to Shoulder problems and their treatment options, Sports Injuries and other orthopedic conditions, visit our YouTube channel Bangalore Shoulder Institute – https://www.youtube.com/@BangaloreShoulderInstitute